PIG Meeting: 29th April 2021
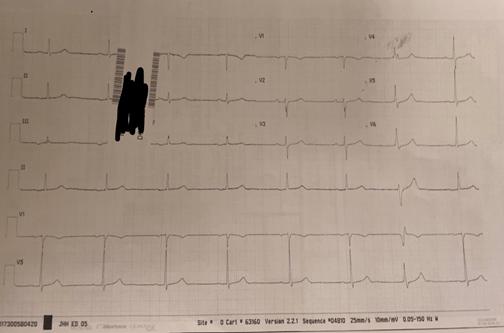
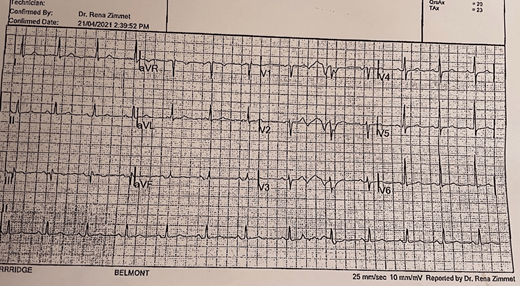
Elective PCI in a man with known triple vessel disease.
Background
- Wheelchair-bound man with muscular dystrophy
- Uses BiPAP at home – for sleep and occasionally daytime (Pressures 19/12cmH20)
- Proceduralist has booked for GA
Issues
- Unable to lie flat, sleeps sitting upright at home. Consideration of ischaemic heart disease contributing to SOB.
- Requires BiPAP if sleeping
- Muscular dystrophy
- Known TVD, Previous PCI with cardiologists only – stented 2 of the 3 vessels. Now proceeding to the third blocked vessel.
Discussion
- Anaesthetic options discussed
- BiPAP required at home, can we administer additional Oxygen via patients own machine?
- Could use HFNP but unlikely to provide enough support given significant pressure on own machine
- Option to borrow a BiPAP machine from ICU
- Consensus that avoidance of a GA in this patient would be preferable
- Uncertain about type of muscular dystrophy but would avoid use of depolarising muscle relaxants
Plan
- Discuss with proceduralist, option for light sedation/no sedation in as elevated position as possible
- BiPAP machine from ICU if needing supplemental O2, consider using own if no O2
- Need some more information on muscular dystrophy and any issues with previous procedure